
Ticagrelor and matching placebo, as well as aspirin and matching placebo, were compounded then over-encapsulated to maintain double-blind conditions. Aspirin and matching placebo were obtained from the University of Iowa Pharmaceuticals (Iowa City, IA). Ticagrelor and matching ticagrelor placebo were provided by AstraZeneca (Wilmington, DE). Block randomization is used in block sizes of six to create groups designed to have equal and balanced sample sizes. Each group received each of three treatments in the crossover study. Study participants were randomized into three groups. 
The aim of this clinical trial is to investigate the effects of ticagrelor on high-shear and low-shear blood viscosity, and explore the effect of ticagrelor on microvascular blood flow in patients with LEAD and type 2 diabetes. The clinical relevance of reducing blood viscosity on microcirculatory perfusion in patients with LEAD remains unknown. Agents that increase adenosine have been shown to lower blood viscosity. The administration of ticagrelor increases adenosine-induced coronary blood flow velocity and improves vascular reactivity compared with clopidogrel. In addition ticagrelor stimulates the rapid release of adenosine triphosphate from red blood cells in vitro. Ticagrelor is potent a P2Y12 receptor antagonist that also inhibits adenosine uptake via the equilibrative nucleoside transporter 1 (ENT1) transporter and increases adenosine concentrations in acute coronary syndrome patients. In contrast, other commonly used therapies such as cilostazol or ticlopidine improve pain-free walking distance, but do not alter blood rheology. Ĭertain pharmacological therapies recommended for the treatment of intermittent claudication in patients with LEAD reduce blood viscosity including clopidogrel and pentoxifylline. Low shear blood viscosity influences microcirculatory flow in patients with LEAD. This phenomenon termed “rheological claudication” was reported in about 25% of patients with moderate to severe claudication and blood hyperviscosity. Elevated blood viscosity is more common in patients with claudication than controls resulting in shorter mean claudication distance. Multiple studies have shown higher blood viscosity values in patients with type 2 diabetes than controls. As compared with non-diabetes patients with LEAD, patients with diabetes have higher rates of severe below-the-knee disease, lower limb amputations and critical ischemia resulting in less effective and durable percutaneous and surgical revascularization rates. Microvascular disease in patients with diabetes and LEAD is associated with more severe major adverse limb events (MALE). Lower extremity arterial disease (LEAD) occurs more often in patients with diabetes than in patients without diabetes. Trial registration Registration number: NCT02325466, registration date: December 25, 2014 Ticagrelor should be considered in the treatment of microvascular disease in patients with LEAD and T2DM. The combination of ticagrelor and aspirin increased MBF in the left foot compared to the other two treatments (p = 0.02), but not in the right foot (p = 0.25). Ticagrelor with or without aspirin reduced low-shear BV by 14.2% and 13.9% respectively, while aspirin monotherapy increased low-shear BV by 9.3% (p < 0.0001). Treatment with ticagrelor with or without aspirin reduced high-shear BV by 5%, in both cases, while aspirin monotherapy increased high-shear BV by 3.4% (p < 0.0001). Use of statins was 93% (high-intensity 43%, moderate intensity 49%), renin–angiotensin–aldosterone system inhibitors (75%) and beta-blockers (61%). The duration of LEAD was 12.3 ± 10.3 years, and 96.9% reported intermittent claudication symptoms. We randomized 70 (45% female) participants aged (mean ± SD) 72 ± 9 years. Randomized, double-blind, double-dummy, crossover trial design that compares treatment with aspirin 81 mg/ticagrelor placebo, aspirin 81 mg/ticagrelor 90 mg twice daily and aspirin placebo/ticagrelor 90 mg twice daily on high-shear (300 s −1) and low-shear (5 s −1) BV, and laser Doppler flowmetry (LDF) in the dorsum of the feet of participants with T2DM. The aim of the trial is to investigate the effects of ticagrelor on BV, and explore the association of BV-dependent MBF in participants with LEAD and type 2 diabetes (T2DM). The contribution of ticagrelor, a P2Y12 antagonist and an adenosine enhancer, on blood viscosity (BV) and BV-dependent MBF in LEAD is unknown.  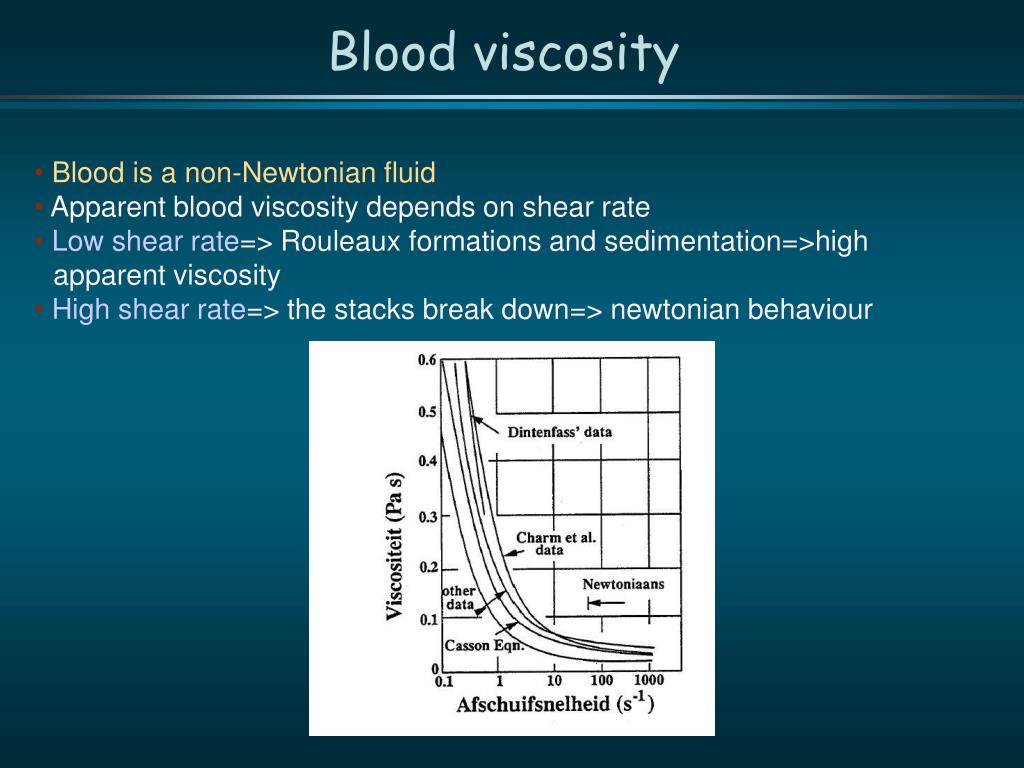
Microvascular blood flow (MBF) impairment in patients with lower extremity arterial disease (LEAD) is associated with more severe major adverse limb events (MALE).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
